Healthcare Billing,
Powered by Intelligent AI
From automated medical coding to real-time eligibility verification ASPRCM Solutions delivers enterprise-grade AI across every step of your revenue cycle management (RCM) workflow, reducing denials and accelerating cash flow.
AI Driven RCM Platform
ASP's technology brings eligibility, coding, claims, and denial management into a single, connected workflow.
By removing silos and automating key processes, the platform improves accuracy, reduces delays, and enables a more predictable path from patient intake to payment.
Proven Performance at Scale
Measurable outcomes across eligibility, coding, and denial management at enterprise scale.
Clinical Intelligence Engine for HCC Coding
A clinical intelligence engine that consistently delivers 97%+ accuracy in HCC coding and does far more than code assignment. With one click, it generates all HCC-qualified codes, MEAT summaries, documentation gaps & queries, annual recapture reports, and clinician review insights so comprehensive that both physicians and payors can rely on it for clinical validation, compliance, and decision-making, without waiting days for chart reviews.
AI Solutions for Every Step of Your Revenue Cycle
End-to-end automation from patient intake through final payment powered by machine intelligence at every touchpoint.
Autonomous Medical Coding
Analyzes clinical documentation and generates codes with up to 95% accuracy across 40+ specialties. Up to 80% of charts are ready to bill, reducing manual effort.
95% Accuracy · 40+ SpecialtiesReal-Time Eligibility & Coverage Intelligence
Verifies coverage across 2,400+ payers, processing up to 180 checks per minute. Helps reduce front-end denials by up to 30%.
2,400+ Payers · 180/minAI-Powered Claim Validation
Applies payer rules and compliance checks before submission. Reduces coding-related denials by up to 40%.
40% Fewer Denials · ComplianceAutomated Payment Posting
Processes ERAs and remittances with minimal manual intervention. Supports faster reconciliation and billing accuracy.
ERA · Auto-ReconciliationAI-Driven AR Optimization
Prioritizes claims using predictive insights and aging analysis. Improves collections and accelerates cash flow.
Predictive · Aging · CollectionsDenial Management & Prevention
Identifies root causes and automates compliant appeal workflows. Helps prevent recurring denials and improve claim success rates.
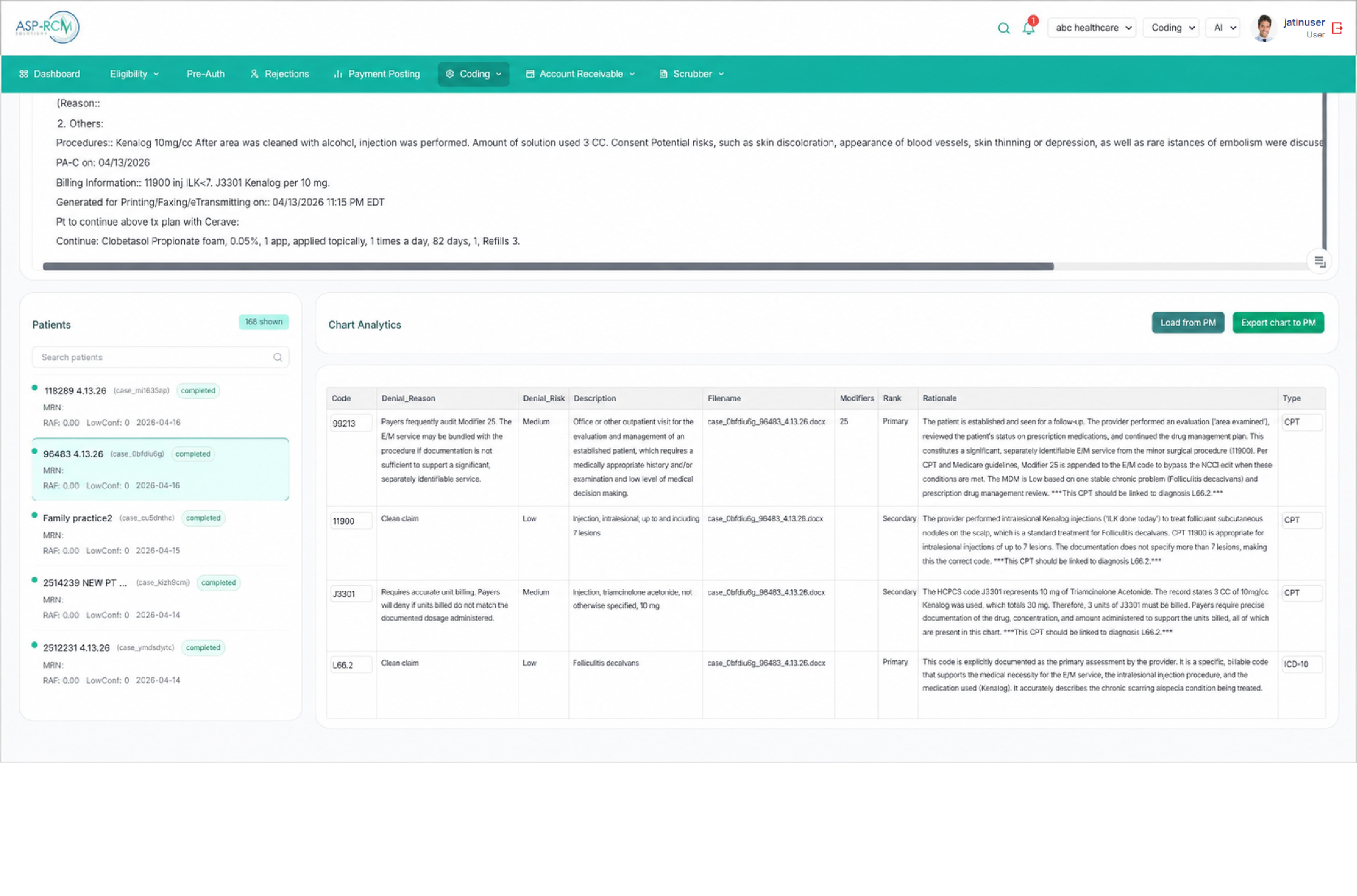
ML Root-Cause · Auto-AppealMedical Coding AI How It Works
Our transformer-based model reads clinical notes, lab results, and operative reports mapping them to precise code sets with up to 95% accuracy across 40+ specialties, processing charts in under 2 seconds. No templates. No guesswork.
End-to-End Revenue Cycle Automated
Every step connected, monitored, and optimized by AI in real time.
Real-Time Analytics & Predictive Intelligence
The platform provides real-time visibility into key revenue cycle metrics, including first-pass rates, denial trends, AR aging, and financial performance.
Built on Enterprise-Grade AI Infrastructure
Purpose-built for healthcare secure, scalable, and designed for continuous improvement.
Results That Speak for Themselves
Measurable outcomes across every client practice, every specialty.
Connects With Your Existing Stack
Seamless EHR, PM, and clearinghouse integrations no rip-and-replace required.























