BLOG • Mar 13, 2026
Hidden Revenue Leaks in Healthcare: How Automation Is Transforming Revenue Cycle Performance
Discover how automation helps healthcare organizations identify hidden revenue leaks, reduce claim denials, and improve revenue cycle management performance.

Hidden Revenue Leaks in Healthcare: How Automation Is Transforming Revenue Cycle Performance

Hidden Revenue Leaks in Healthcare: How Automation Is Transforming Revenue Cycle Performance
In today’s complex healthcare financial environment, many healthcare organizations unknowingly lose millions each year due to revenue leakage across the revenue cycle. From coding errors in healthcare billing and documentation gaps to claim denials and eligibility issues, small operational inefficiencies can quietly erode hospital revenues.
Industry research indicates that healthcare organizations typically lose 3–5% of net patient revenue due to revenue leakage, which for a mid-sized hospital can translate into $15–$25 million in lost revenue annually.
For C-suite executives and Revenue Cycle Management (RCM) leaders, these losses directly impact critical financial metrics such as:

Addressing these inefficiencies has therefore become a strategic priority for healthcare organizations seeking to improve healthcare revenue cycle optimization and long-term financial sustainability.

Understanding Where Revenue Leakage Occurs
Revenue leakage can occur at multiple stages of the Revenue Cycle Management Process, including patient intake, clinical documentation, medical coding, claims submission, and payer reimbursements.
Common sources of revenue leakage include:
• Coding errors in healthcare billing
• Inefficient claim denial management processes
• Eligibility verification and authorization issues
• Documentation gaps in clinical records
• Underpayments from insurance payers
• Manual billing workflows and operational inefficiencies
Industry benchmarks highlight the scale of these challenges:
• 5–10% of medical claims are denied on first submission
• 60–70% of denied claims are never reworked
• 80–90% of claim denials are preventable
As a result, hospitals can lose 1–3% of net patient revenue due to claim denials alone.

Revenue Leakage Breakdown Across the Revenue Cycle
Revenue leakage rarely stems from a single issue. Instead, it typically occurs across several operational areas within the revenue cycle.
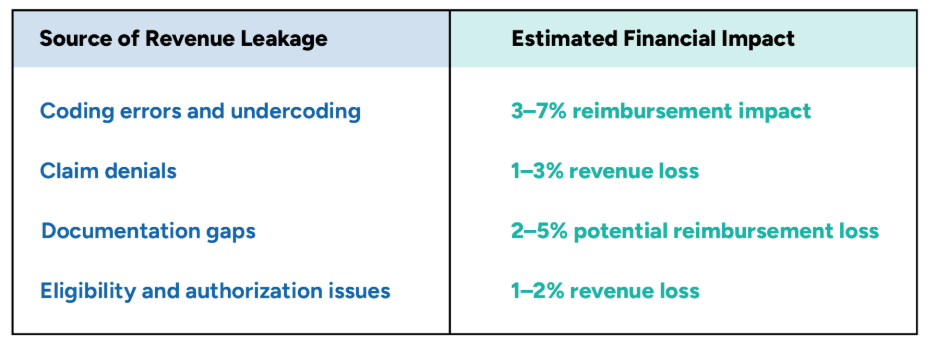
For healthcare organizations operating at scale, even modest inefficiencies in these areas can translate into millions of dollars in lost revenue annually.

Coding Accuracy and Documentation Challenges
Coding accuracy plays a crucial role in ensuring appropriate reimbursement. However, many healthcare organizations still rely heavily on manual coding workflows that increase the risk of errors.
Industry benchmarks show:
• Manual coding environments typically achieve 90–95% coding accuracy
• 5–10% of medical charts may contain coding errors
• Undercoding alone can reduce reimbursement by 3–7%
Documentation gaps further contribute to revenue leakage.
Studies indicate:
• 15–25% of medical records contain documentation gaps
• 10–15% of diagnoses may be missing from claims submissions
These issues can lead to inaccurate DRGs, missed diagnoses, compliance risks, and reduced reimbursement.

Eligibility and Authorization Errors
Front-end revenue cycle processes also play a significant role in revenue leakage.
Industry data shows:
• 20–30% of claim denials are related to eligibility issues
• 10–20% of healthcare claims require prior authorization
Without automated eligibility verification systems, these errors often result in claim delays, denials, and unnecessary administrative workload.

How Automation Reduces Revenue Leakage
Healthcare organizations are increasingly adopting automation in healthcare revenue cycle management to address operational inefficiencies.
Automation technologies help streamline workflows, reduce manual errors, and improve billing accuracy across the revenue cycle.
Automation solutions help healthcare organizations:
• Identify coding inconsistencies before claims submission
• Automate eligibility verification and authorization checks
• Improve claim denial management processes
• Enable automated claim scrubbing
• Detect underpayments from insurance payers
Industry studies show automation can deliver measurable improvements:
• 30–50% reduction in preventable claim denials
• 10–20% reduction in AR days
• 30–40% reduction in administrative effort
These improvements significantly enhance revenue cycle efficiency and financial performance.

How ASPRCM Solutions Helps Healthcare Organizations
At ASPRCM Solutions, we combine advanced technology, AI-driven automation, and experienced revenue cycle specialists to help healthcare organizations eliminate hidden revenue leakage and optimize revenue cycle performance.
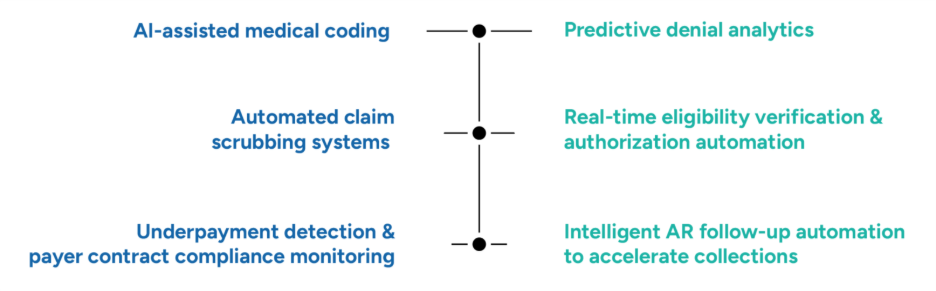
Our technology-enabled RCM solutions focus on:
• AI-assisted medical coding to improve coding accuracy and documentation quality
• Predictive denial analytics to identify denial patterns and prevent claim rejections
• Automated claim scrubbing systems to detect claim errors before submission
• Real-time eligibility verification and authorization automation
• Underpayment detection and payer contract compliance monitoring
• Intelligent AR follow-up automation to accelerate collections
By integrating technology with expert RCM operations, ASPRCM enables healthcare organizations to strengthen financial performance while reducing operational complexity.

Business Value Metrics (BVM): Pre vs Post Automation Impact
Healthcare organizations implementing automation-driven RCM solutions often see measurable improvements in key financial and operational metrics.

These improvements translate directly into faster reimbursements, improved cash flow, and stronger financial visibility for healthcare leadership.
Key Takeaways for Healthcare Leaders
Healthcare organizations are increasingly recognizing revenue cycle efficiency as a strategic driver of financial performance. Key insights for healthcare executives include:
• Revenue leakage can account for 3–5% of net patient revenue, representing millions of dollars in potential losses annually.
• Claim denials remain one of the largest contributors to revenue leakage, with up to 80–90% of denials being preventable through improved processes and automation.
• Coding inaccuracies and documentation gaps continue to impact reimbursement accuracy and compliance across healthcare organizations.
• Automation and AI-driven RCM solutions can significantly reduce operational inefficiencies, improve coding accuracy, and accelerate reimbursement cycles.
• Healthcare organizations implementing intelligent RCM automation are seeing 30–50% reductions in preventable denials and faster collections.
For healthcare leaders, investing in automation-driven revenue cycle strategies is becoming essential to improving financial sustainability and operational efficiency.

Conclusion
Revenue leakage remains one of the most significant financial challenges facing healthcare organizations today. From coding errors and documentation gaps to claim denials and eligibility issues, inefficiencies across the revenue cycle can quietly erode millions in revenue each year.
However, by adopting automation in healthcare revenue cycle management, healthcare organizations can significantly reduce these inefficiencies and improve financial performance.
With the right combination of technology, automation, and expert revenue cycle management support, healthcare organizations can minimize revenue leakage, accelerate reimbursements, and build a more efficient and financially resilient healthcare system.
Share your details with us, and we'll set up a tailored demo just for you.

Hidden Revenue Leaks in Healthcare: How Automation Is Transforming Revenue Cycle Performance
BLOG • Mar 13, 2026
Hidden Revenue Leaks in Healthcare: How Automation Is Transforming Revenue Cycle Performance